

Jeanne Catherine & Adriaan Denkers, PhD
January 31, 2023
Jeanne is the co-founder, COO, and lead scientist of Innate Health ResearchAdriaan is the senior research scientist and advisor at Innate Health Research.
Introduction
Substance use disorder (SUD) constitutes a large societal problem. The 2019 National survey on drug use and health revealed that 60.1% of Americans (older than 12 years) reported to have used drugs during the last month1. In 2019, more than 70.000 Americans died from a drug overdose2. The annual cost related to SUD in United States hospitals alone was estimated at $13.2 billion (Peterson et al, 2021). Helping individuals cope with and potentially overcome their addictions, is essential for societies, communities, families, and individuals involved.
State of the field
The standard treatment for SUD’s involves Cognitive Behavioral Therapy (CBT) in combination with Medicine Assisted Treatment (MAT). Research results generally do suggest that such treatment helps to reduce drugs or alcohol intake (Ray, et al., 2020; Magill et al., 2019). MAT has been found to reduce the intake of drugs and alcohol (Manhapra et al., 2018; Nielsen et al., 2016; O’Connor et al., 2020). Nonetheless, the efficacy of traditional CBT in the treatment of SUD’s is much discussed. One reason for this discussion is that CBT does not appear to systematically outperform the other specific treatments – not refuting that CBT does render better results than no treatment (Hunt et al., 2019).
These less-than-optimal results regarding CBT on SUD might be due to the specificity of CBT treatment. Substance use disorders tend to go hand in hand with other psychiatric disorders, especially depression and anxiety. Ample documentation exists that comorbidity is a rule rather than an exception among individuals suffering from a substance or alcohol use disorder: both in substance abuse treatment settings (e.g., Brems & Johnson, 2004; Havassy, Alvidrez & Owen, 2004; Wolitzky-Taylor et al.,2022) and in the general population (e.g., Kessler et al., 1997; National Institute on Alcoholism and Alcohol Abuse, 2006; Substance Abuse and Mental Health Services Administration, 2005). A CBT therapy that specifically focusses on reducing the SUD, is unlikely to effectively reduce other psychiatric issues.
Besides the standard treatment the field shows many different alternative types of treatment, among which group therapies (Lo Coco et al., 2019), the 12-step programs (Kelly et al., 2020), mindfulness (Zgierska et al., 2009), Acceptance and Commitment Therapy (A-Tjak, 2015), non-invasive brain stimulation (Petit et al., 2022), and the seven challenges program (Parisi et al., 2021). Although the body of knowledge on the effects of such interventions is growing, the results are still unclear and mixed.
Innate health interventions
Recently, innate health (Catherine et al.,2022) or the three principles intervention has entered the field of substance or alcohol use disorders (SUD / AUD) and treatment. A handful of rehabilitation centers have embraced this approach and incorporated it into their treatment of clients. Judging on the reviews, clients appear to be enthusiastic.
These innate health programmes are typically based on the work of Sydney Banks (see his book: The Enlightened Gardener) and aim to promote awareness of one’s own well-being, potential for innate resilience, and capacity for clearer thinking. Facilitators deliver the program to groups over a series of sessions or days, in this case daily for 28 days, and team members provide insightful, non- judgemental conversations, delivered with love. Discussions include topics about the human psychological experience, such as feeling stuck in repetitive, spiralling, anxious, depressive, or compulsive thinking and how one’s own thinking is likely to be observed by each individual as a single objective truth. Activities include building thought awareness, modelling non-judgmental observation, and consciously experiencing the results of a quiet state off mind (i.e., inspiration, intuition, and wisdom).
Research into the effects of innate health-based interventions show promising results within different fields. Innate health interventions have shown to be related to increased levels of wellbeing and/or decreased levels of distress within organizations (Borg, 1997; Roy, 2007), communities (Mills, 2005a, 2005b), prison rehabilitation settings (Catherine et al., 2022; Kelley et al., 2018; Kelley et al., 2021; Kelley et al., 2019) and among first-year nursing students (Sedgeman, 2008) and female Somali refugees (Robertson et al., 2019).
Hypotheses
The results are expected to indicate that:
- The program leads to less addiction and more mental health
- Medication is expected to (partly) explain the reduction of addiction
- Innate health, therapeutic alliance and resilience are expected to explain reduction in addiction (above MAT) and improved mental health
The study will control for social desirability. Because few comparable studies include social desirability, no hypotheses are formulated concerning change in social desirability and the influence of this bias on the results.

Method
Procedure
Our research team was asked to assess anonymized client data collected by a residential rehabilitation center for addictions located in the northeastern region of the United States. Following the HIPAA privacy rules, this entity invited clients to fill out three digital questionnaires: at entrance (after detox), at departure from the center, and two months following departure. Clients could decline to participate at any time. All information collected was processed anonymously and completely de-identified with the specific intent to evaluate center programming. In this study, only the first two of these questionnaires have been used, because too few participants filled out the last questionnaire.Method
Procedure
Our research team was asked to assess anonymized client data collected by a residential rehabilitation center for addictions located in the northeastern region of the United States. Following the HIPAA privacy rules, this entity invited clients to fill out three digital questionnaires: at entrance (after detox), at departure from the center, and two months following departure. Clients could decline to participate at any time. All information collected was processed anonymously and completely de-identified with the specific intent to evaluate center programming. In this study, only the first two of these questionnaires have been used, because too few participants filled out the last questionnaire.
Participants
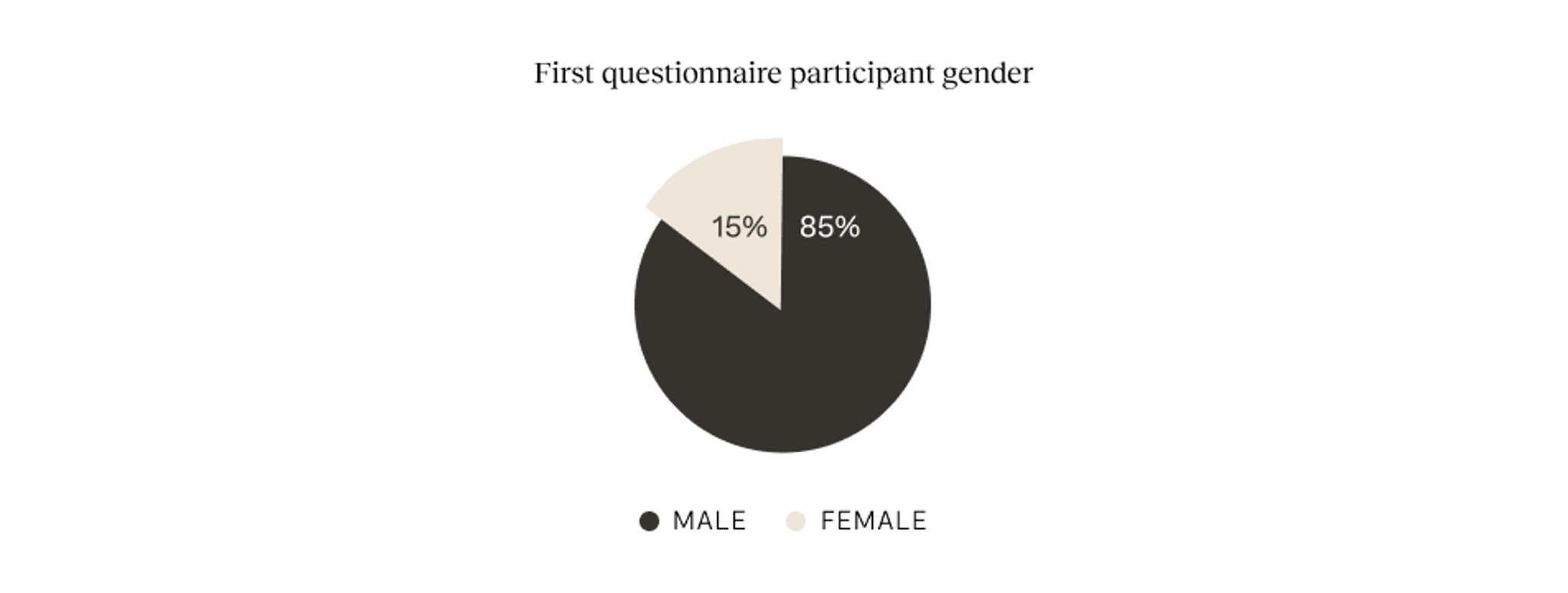
The first questionnaire was filled out by 166 participants, of which 24 (15%) were female and 142 (85%) were male. The average age was 38 years, +/- 11.7. Of the participants, 15 (9%) mentioned having ever served in the military. The majority reported to be unemployed, 79 (48%) were looking for work and 12 (7%) were not looking for work; 39 (24%) and 13 (8%) reported to have full- or part-time employment; 22 (13%) reported to be disabled, 5 (3%) self-employed, 2 (1%) retired and 2 (1%) student. The second questionnaire was filled out by 105 participants, of which 12 (11%) reported to be female and 94 male. At Time 2, the average age remained 37 years, +/- 11.2. At entrance into the center, the majority of participants had been located at Queen City (of which, 59 at Manchester Detox, 58 at Manchester Monitoring Unit, 12 at the Respite Unit and 8 at Manchester Woman’s Residential); 38 were located at Webster Franklin Place, 15 at Ray House and 1 Out Patient. At departure 105 participants had filled out a questionnaire. We were able to couple almost all the participants that filled out the second questionnaire to their first questionnaire: 104 participants filled out both questionnaires.
Measurements
The participants answered questions related to nine different concepts: distress, well-being, drug use, commitment to sobriety, medical assisted treatment (MAT), therapeutic alliance, resilience, innate health and social desirability.
Table 1 shows the reliabilities of these concepts both at entrance and at departure. This table shows that all these concepts have been measured reliably.
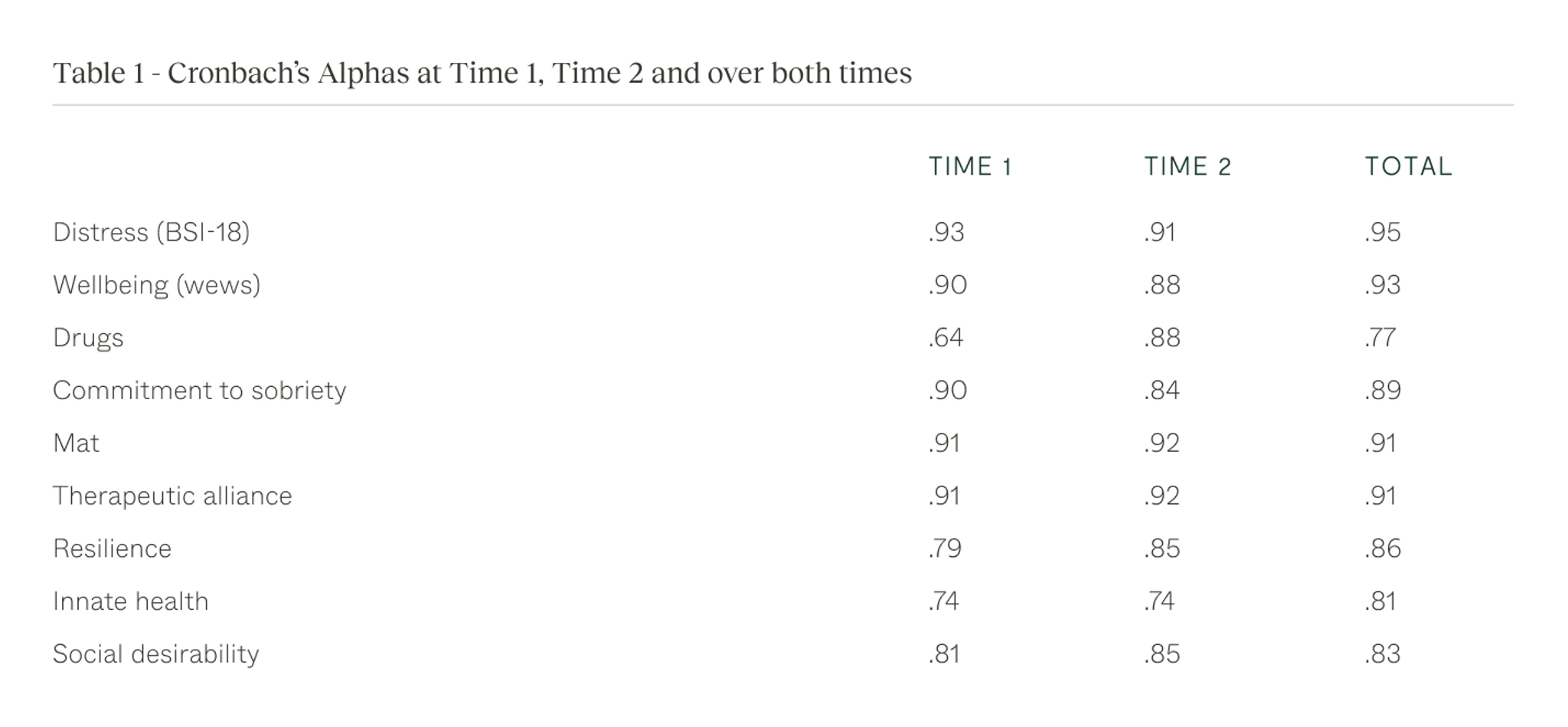

Psychological distress was measured with Brief Symptom Inventory which consists of 18 items, of which six are on anxiety, six on depression and sixon somatization. This shortened form of the BSI instrument gathers data to measure psychological distress and psychiatric disorders in medical and community populations (Derogatis, 1993; 2001; Derogatis & Melisaratos, 1983). The BSI-18 has found to have good psychometric (Meijer, et al., 2011).
The Warwick-Edinburgh Well-Being Scale-Short form (Tennant et. al., 2007) was developed at the Universities of Warwick and Edinburgh and comprises seven-items that relate to an individual’s state of mental well-being (thoughts and feelings) in the previous two weeks. The WEMWBS has good psychometric properties (Tennant et al., 2007). Each item is worded positively and together they cover most, but not all, attributes of mental well-being including both hedonic and eudemonic perspectives.
Other programming offered to people struggling with home insecurity include:
- Housing first interventions: Effective for stabilizing housing, however, do not appear to systematically improve quality-of-life, physical and/or mental health, and/or reduce substance use (Aubry, et al., 2020).
- Occupational therapy: In an embryonic stage and does not show a clear picture of results yet (Marshall et al., 2020).
- Relaxation response training: May be effective in improving anxiety and mental health status
Conclusion
The current study offers the first scientific support for the notion that innate health interventions may be beneficial to individuals suffering from addictions. These results may encourage centers that are considering incorporating innate health into their program and may provide support for those that already have incorporated this approach. This approach may help diminish the large societal problem of substance use disorder by offering effective treatment and thus reducing the enormous cost in care and human lives caused by addictions. This would be beneficial to the individuals involved, their family and friends, the communities in which they live, and societies as a whole.
Acknowledgements
This work was supported by the Three Principles Research & Consulting (3PRC).
References
A-Tjak, J.G.L., Davis, M.L., Morina, N., Powers, M.B., Smits, J.A.J., & Emmelkamp, P.M.G. (2015). A Meta-Analysis of the Efficacy of Acceptance and Commitment Therapy for Clinically Relevant Mental and Physical Health Problems. Psychotherapy and Psychosomatics, 84(1), 30 – 36. DOI10.1159/000365764.
Bentzley, B.S., Han, S.S., Neuner, S. Humphreys, K., Kampman, K.M., & Halpern, C.H. (2021). Comparison of Treatments for Cocaine Use Disorder Among Adults A Systematic Review and Meta-analysis. JAMA Network Open, 4(5), Article Number: e218049. DOI: 10.1001/jamanetworkopen.2021.8049
Berman, A.H., Palmstierna, T., Källmén, H., Bergman, H. (2007). The self-report Drug Use Disorders Identification Test—Extended (DUDIT-E): Reliability, validity, and motivational index. Journal of Substance Abuse Treatment, 32, 357– 369
Brems, C., & Johnson, M. E. (2004). Comorbidity in Alaska: Evidence and implications for treatment and public policy. Alaska Medicine, 46, 4-19.
Bressler, S.L., & Seth, A.K. (2011). Wiener-Granger Causality: A well established methodology. Neuroimage, 58(2), 323-329.
Catherine, J., Denkers, A., & McGinty, A. (2022). Innate Health: A Novel Examination of What Explains Well-being, Prosocial Behavior, and Aggression among Men Living in a UK Prison. Preprints, 2022060023 (doi: 10.20944/preprints202206.0023.v1). Under review.
Calomarde-Gomez, C., Jimenez-Fernandez, B. Balcells-Olivero, M., Gual, A., & Lopez-Pelayo, H (2021). Motivational Interviewing for Cannabis Use Disorders: A Systematic Review and Meta-Analysis. European Addiction Research (Early Access). DOI: 10.1159/000515667
Collaborate with Innate Health Research
We work closely with practitioners, academics and funders to provide research-backed evidence for innate health. If you’d like to work with us on a project, please get in touch

Join the movement
Sign up to gain access to webinars, current evidence, and conversations about researching your programs.



